Imagine your kidneys as a sophisticated coffee filter. Their job is to keep the good stuff-like proteins-in your blood while letting waste and extra water pass through as urine. When that filter gets damaged or leaky, those proteins slip through. That is exactly what happens with Proteinuria is a condition where an unusually high amount of protein is found in the urine . While it might sound like a minor detail, seeing protein in your urine is often the first red flag that your kidneys are struggling. If you catch it early, you can stop the leak; if you ignore it, you risk permanent kidney failure.
The Warning Signs: Is Your Urine Trying to Tell You Something?
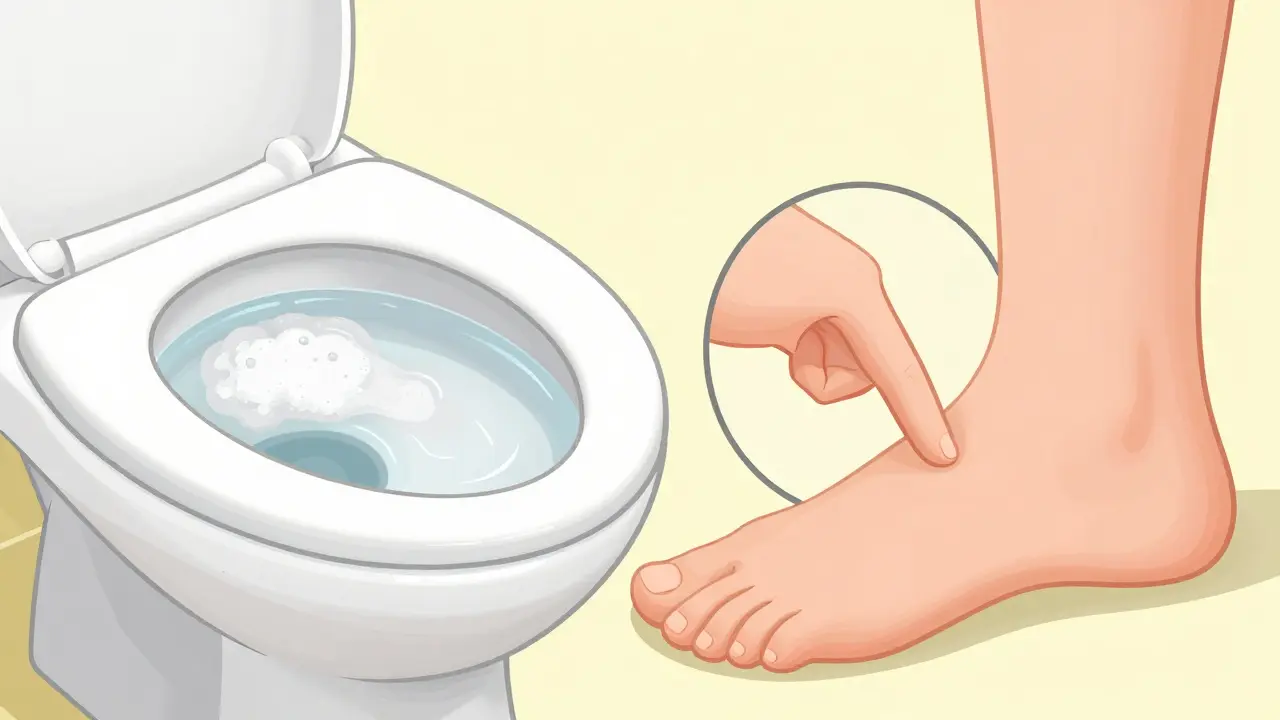
For many people, the early stages of proteinuria are completely silent. You can't "feel" protein leaving your body. However, once the leak becomes significant-usually when you're losing more than 1,000 mg of protein a day-your body starts sending loud signals. The most common sign is foamy or bubbly urine. If your urine looks like the top of a cappuccino or has a layer of bubbles that doesn't disappear after flushing, it's a classic sign of excess protein.
As the condition progresses, you might notice Peripheral Edema, which is just a medical way of saying swelling. This usually hits the ankles, feet, and around the eyes. Why? Because proteins like albumin act like magnets for water in your blood vessels. When you lose too much protein in your urine, water leaks out of your blood and into your tissues, causing that puffy look. Other signs include feeling unusually tired, muscle cramps at night, or even nausea if the buildup of waste in your blood becomes too high.
Why Is Protein Leaking? Understanding the Causes
Not every positive protein test means you have kidney disease. Sometimes, it's just a temporary glitch. This is called transient proteinuria. You might see protein in your urine if you've had a high fever, went through an intense workout, or are severely dehydrated. Even extreme emotional stress or very cold weather can cause a temporary spike. In these cases, the "leak" fixes itself once the trigger is gone.
The real concern is persistent proteinuria, where the protein is always there. The most common culprit is Diabetic Nephropathy, which accounts for about 40% of chronic cases. High blood sugar damages the kidney's delicate filters over time. Following closely is hypertension, or high blood pressure, which puts too much pressure on the renal vessels, forcing protein through the filter. Other causes include autoimmune diseases like lupus, where the immune system mistakenly attacks the kidneys, or conditions like preeclampsia during pregnancy.
How Doctors Detect and Measure the Leak
Detection usually starts with a simple dipstick test during a routine check-up. It's fast, but it's not always accurate. Think of it as a "yes or no" test. To get the real story, doctors use more precise methods to figure out exactly how much protein is escaping.
| Test Type | How it Works | Accuracy/Use Case |
|---|---|---|
| Dipstick Test | Chemical strip changes color | Fast screening; lower precision |
| UPCR / UACR Spot Test | Ratio of protein to creatinine in one sample | High correlation with 24-hour tests |
| 24-Hour Collection | Collecting all urine for a full day | Gold standard for precise quantity |
| Electrophoresis | Separates proteins by size/charge | Used to find specific proteins (e.g., Bence-Jones) |
A key metric you'll hear about is the Urine Protein Creatinine Ratio (UPCR). Because urine concentration changes depending on how much water you drink, doctors compare the protein to creatinine (a waste product that stays steady). If your UPCR is consistently above 50 mg/mmol, it usually signals a need for a deeper dive into your kidney health.
Strategies to Reduce Protein Leak and Protect Kidneys
The goal of treatment isn't just to stop the protein from leaking; it's to stop the damage that's causing the leak. Once you reduce proteinuria, you significantly lower your risk of ending up on dialysis. For every 50% reduction in protein excretion, the risk of progressing to end-stage renal disease drops by about 30%.
Medication is often the first line of defense. Drugs like ACE inhibitors or ARBs are commonly prescribed. Even if you don't have high blood pressure, these meds are great because they relax the pressure inside the kidney's filters, reducing protein loss by 30-50%. For those with diabetes, newer drugs called SGLT2 inhibitors have shown a massive impact, slowing the decline of kidney function by about 30%.
Dietary changes can also make a huge difference. Eating too much protein can actually put more strain on your kidneys. A low-protein diet-roughly 0.8g of protein per kilogram of body weight-can help reduce the workload on your filters. Pairing this with high-fiber foods and keeping your blood pressure below 130/80 mmHg can further slash protein excretion by 20-40%.
What to Expect During Long-Term Management
Managing kidney health is a marathon, not a sprint. If you've been diagnosed with persistent proteinuria, you'll likely be on a regular monitoring schedule. For high-risk groups like diabetics, this might mean a protein check every three months. The target is usually a 30% reduction from your starting baseline within the first 90 days of treatment.
It's also important to be your own advocate. Keep an eye on your ankles for swelling and notice if your urine becomes more foamy. These small changes are often the first signs that your treatment needs adjusting or that your blood pressure is spiking. While some medications like ACE inhibitors can cause a dry cough-leading some people to stop taking them-be sure to talk to your doctor about alternatives rather than just quitting, as these drugs are vital for kidney protection.
Can I have protein in my urine if I'm healthy?
Yes, this is called transient proteinuria. It can happen due to fever, intense exercise, or dehydration. In these cases, it's temporary and doesn't indicate kidney disease. However, if it persists across multiple tests, it requires medical investigation.
Does foamy urine always mean kidney damage?
Not necessarily, but it is a strong indicator. While some foams are just caused by the speed of the urine stream or certain cleaners in the toilet bowl, persistent, thick foam is often caused by albumin leaking into the urine. You should get a simple dipstick test to confirm.
What is the difference between proteinuria and albuminuria?
Proteinuria is a general term for any protein in the urine. Albuminuria is a specific type of proteinuria where albumin-the main protein in your blood-is the one leaking. Because albumin is the most critical marker for kidney health, doctors focus on it most heavily.
Can a low-protein diet really fix the leak?
It doesn't "fix" the filter, but it reduces the pressure on it. By limiting protein intake to about 0.6-0.8g/kg of body weight, you reduce the amount of protein the kidney has to process, which can decrease protein excretion by 15-25% and slow the progression of kidney damage.
How dangerous is it to lose 1g of protein a day?
Losing more than 1g of protein daily is a serious clinical sign. Studies show that without intervention, people with this level of protein loss have a roughly 50% risk of developing end-stage renal disease within 10 years. This makes aggressive treatment with blood pressure and glucose management essential.
Next Steps for Your Health
If you've noticed symptoms like swelling or foamy urine, the first step is a simple urinalysis at your GP's office. For those already managing a condition, the goal is to maintain a stable UPCR and keep blood pressure strictly controlled. If you are on a protein-restricted diet, consider working with a renal dietitian to ensure you're still getting enough nutrients to prevent malnutrition while protecting your kidneys.

Comments
Glad someone finally explained the foamy urine thing in plain English.
It's absolutely typical for the mainstream medical establishment to push these so-called 'gold standard' 24-hour collections while completely ignoring the fact that the very chemicals used in dipstick tests are likely designed by the same corporate conglomerates that profit from the dialysis machines they're scaring us into needing, and honestly, if you actually look into the history of renal medicine, you'll find that the push for ACE inhibitors is just a way to keep the population in a state of permanent chemical dependency while they ignore the real environmental toxins leaching into our groundwater that are actually causing the filter failure in the first place, and don't even get me started on the 'low protein' diet which is basically just a way to make us weak and compliant while the pharmaceutical giants laugh all the way to the bank with their SGLT2 inhibitors that probably have side effects they're not even telling us about in the clinical trials.
Um, actually, the UPCR is way more reliable than a basic dipstick and anyone who thinks otherwise is just delusional 🙄 I've seen people ignore their bubble urine for months and then act shocked when their creatinine spikes! Like, hello?? Use your brain!! 💅✨
everyone just ignores the blood pressure part but that's literally the whole game... if you dont hit that 130/80 your kidneys are basically just ticking time bombs
medical logic is just a cycle of damage and patch work. protein leak is just the symptom not the cause. typical
It's wild how we treat the body like a machine with filters instead of a living system. I guess the metaphor works, but the stress of monitoring these numbers can sometimes be as bad as the condition itself.
One must contemplate the profound irony that the very sustenance we seek through protein may become the catalyst for our bodily decline. It is a reminder of the delicate equilibrium required to maintain human existence.
Who cares about the 24 hour test? Just pee in a jar and hope for the best! This whole guide is just a fancy way of saying your kidneys are leaking like a rusty pipe in an old Delhi apartment!
Oh my goodness, this is such an important reminder for everyone to take care of their health! 🌟 Please don't be scared if you see some bubbles, just go get a check-up and stay positive because catching things early is a total game-changer and we can all get through this with the right support and a little bit of dietary magic! 🌈💪✨ Keep fighting for your health everyone, you've got this!!
Right, because nothing says 'health' like a 24-hour urine collection. Truly the highlight of any adult's week.
Big Pharma loves pushing those ACE inhibitors. Just another way to keep you on a pill for life while they ignore the ancestral diets that actually worked before everything was processed garbage.
I really appreciate the mention of the renal dietitian. It's so easy to accidentally under-eat when you're restricting protein.
The idea of my kidneys just 'leaking' is absolutely terrifying! I can't even imagine the stress of seeing those bubbles for the first time! 😱
It's great that we're sharing this information. Everyone's journey with kidney health is different, but having these tools helps us all feel more included in our own care. Let's support each other in making these lifestyle changes!