Medication Formulation Side Effect Comparison Tool
Understand Your Medication Options
This tool compares common side effects between immediate-release (IR) and extended-release (ER) versions of medications. Based on research in the article, ER formulations often reduce side effects by smoothing drug peaks in your bloodstream.
Select a medication and click "Compare Side Effects" to see side effect differences
When you pick up a prescription, you might not think about whether it’s a tablet, capsule, or extended-release version. But the form you take can change how your body handles the drug - and even how you feel while taking it. A simple switch from immediate-release to extended-release can cut your side effects in half. Or it could make swallowing the pill a daily struggle. Understanding these differences isn’t just about science - it’s about making your medication work better for you.
Tablets vs Capsules: What’s Really Different?
At first glance, tablets and capsules look similar. Both are solid oral doses you swallow with water. But how they behave inside your body? Very different.
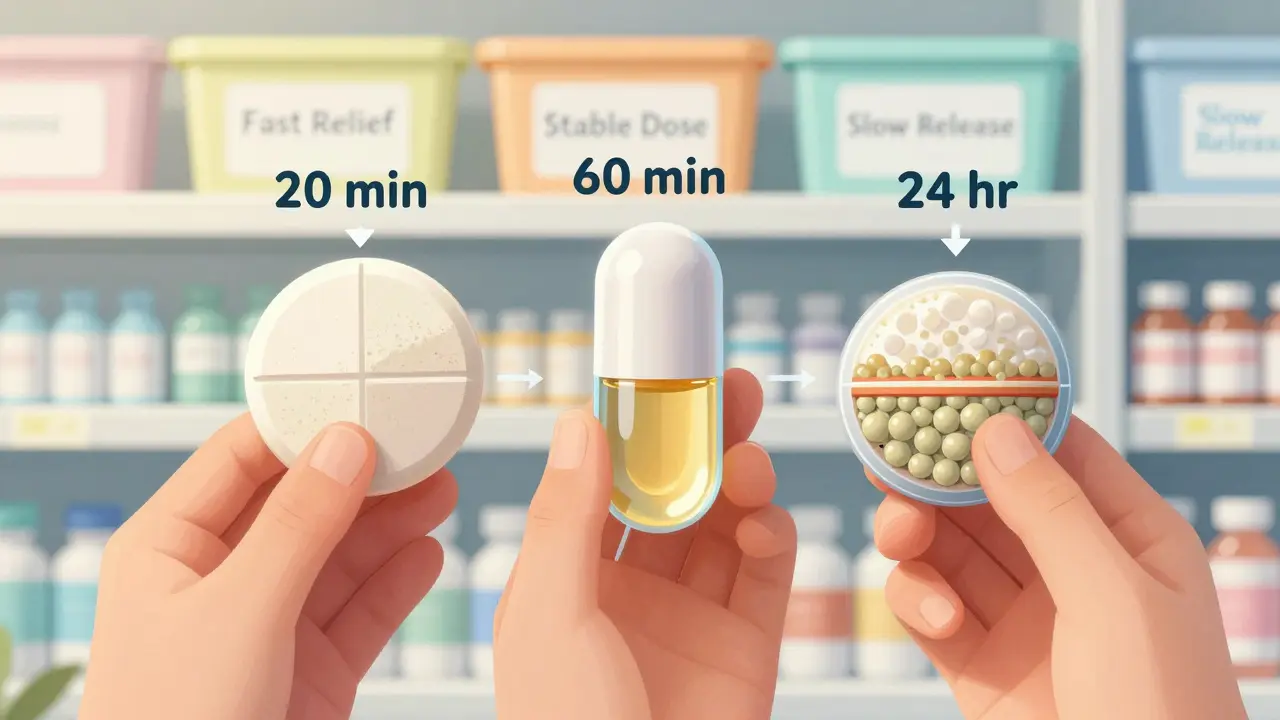
Tablets are compressed powders, often with binders, fillers, and coatings. They take longer to break down - usually 30 to 60 minutes in the stomach. That’s why their peak effect often comes 1 to 2 hours after taking them. Their big advantage? Stability. A tablet can sit on your shelf for 2 to 3 years without losing strength. That’s why pharmacies stock them in bulk.
Capsules, on the other hand, are gelatin or plant-based shells filled with powder or liquid. They dissolve faster - often in under 20 minutes. That means faster absorption. Studies show capsules deliver the drug into your bloodstream 20% to 30% quicker than tablets. That’s why some painkillers or antibiotics come in capsules: you want the relief fast.
But there’s a trade-off. Capsules don’t last as long on the shelf. Moisture and heat can degrade the contents. That’s why you’ll often see them in blister packs, not bottles. And if you’re sensitive to gelatin, plant-based capsules are now common - but they still cost more.
Extended-Release: Slower Release, Fewer Side Effects
Extended-release (ER), also called sustained-release (SR) or extended-duration (XR/XL), isn’t just a slower pill. It’s a carefully engineered system designed to release the drug over 12 to 24 hours. Think of it like a tiny time-release capsule inside your body.
How does it work? There are four main methods:
- Hydrophilic matrix: Uses a gel-forming material like HPMC (hydroxypropyl methylcellulose). When it hits stomach fluid, it swells into a gel that slowly lets the drug leak out. Common in ER versions of metformin and gabapentin.
- Hydrophobic matrix: Uses waxy or plastic polymers like ethylcellulose. The drug must diffuse through tiny pores. Used in some ER opioids and antidepressants.
- Reservoir system: The drug is sealed in a plastic shell with a tiny hole. Pressure pushes the drug out at a steady rate. Found in some blood pressure pills.
- Osmotic system: Uses water to build pressure inside the tablet, forcing drug out through a laser-drilled hole. Used in drugs like OxyContin and Concerta.
The result? Instead of a spike in drug levels followed by a crash, you get a steady flow. That’s why extended-release versions often cause fewer side effects.
How Side Effects Change With Formulation
Side effects aren’t random. They’re often tied to how high the drug spikes in your blood. High peaks = more nausea, dizziness, headaches.
Take bupropion (Wellbutrin). The immediate-release version causes nausea in about 19% of users. The extended-release version? Just 13%. Dizziness drops from 25% to 18%. Why? The ER version avoids the sharp highs that trigger those reactions.
Same pattern with venlafaxine (Effexor). ER reduces nausea by 18% and dizziness by 22% compared to the immediate-release form. A 2017 review of 15 studies found that extended-release versions of epilepsy drugs cut side effects by 25% to 40%.
But here’s the catch: ER doesn’t eliminate side effects. It just spreads them out. And for some people, the slow release causes new problems.
For example, if you have slow digestion - like with gastroparesis or after gastric surgery - the ER pill might sit in your stomach too long. In 5% to 10% of these cases, the drug doesn’t release properly. That means you get no benefit… or worse, a delayed overdose if it finally dumps all at once.
And you can’t crush or split an ER pill. Ever. Doing so can cause a dangerous rush of medication. One patient taking ER oxycodone and crushing it ended up in the ER with respiratory failure. That’s why ER pills are often larger and harder to swallow.
Who Benefits Most - And Who Should Avoid ER?
Extended-release formulations shine for people taking daily meds for chronic conditions. Think depression, epilepsy, high blood pressure, or ADHD.
A 2022 case study showed a bipolar patient improved from 65% adherence with three daily doses to 92% with one daily ER dose. Mood episodes dropped by 47%. That’s not just convenience - it’s life-changing.
But ER isn’t for everyone.
- Older adults: 27% of negative reviews mention trouble swallowing large ER tablets. A 2022 Mayo Clinic survey found 1 in 4 elderly patients struggle with them.
- People with GI issues: If you have Crohn’s, gastroparesis, or recent abdominal surgery, ER may not absorb right. Your doctor should avoid prescribing them.
- Those needing dose flexibility: ER pills come in fixed strengths. If you need to adjust your dose by 25 mg, you’re stuck. Immediate-release lets you cut pills or take half-doses.
Also, cost matters. ER versions often cost 2 to 3 times more than immediate-release. Generic bupropion costs $15/month. Wellbutrin XL? $185. That’s why many patients switch back - even if side effects return.
Label Confusion and Hidden Risks
Ever seen a pill labeled “SR,” “XR,” “CR,” or “XL”? They all mean different things.
- SR (Sustained-Release): Releases over several hours. Not always 24-hour.
- ER/XR/XL (Extended-Release): Usually 12-24 hours. Most common today.
- DR (Delayed-Release): Coated to survive stomach acid. Releases in the intestine. Like enteric-coated aspirin or valproate.
Confusing them can be dangerous. A 2021 analysis found 12% of medication errors involved mixing up ER and immediate-release versions. One patient took ER amphetamine thinking it was immediate-release - and overdosed.
Always check the label. If it says “extended-release,” don’t assume it’s the same as the regular version. Even if they have the same generic name.

The Future: Smarter, Personalized Delivery
The next wave of drug delivery is getting smarter. Rytary, approved in 2023, uses three-part pellets that release levodopa in pulses - mimicking natural brain chemistry in Parkinson’s. It cuts “off” time by over 2 hours a day.
Researchers are testing gastric-retentive systems that stay in the stomach for 24 hours. Others are building pH-sensitive coatings that release only in the colon - perfect for drugs that irritate the stomach.
But challenges remain. Polymer-based coatings from ER pills are now showing up in wastewater. A 2022 study found them in 78% of samples. That’s a new environmental concern.
And regulatory standards are tightening. The FDA now requires strict tests to prove ER pills work the same across all patients - young, old, healthy, or sick. Not all do.
What You Should Do
- If you’re on a daily medication and have side effects like nausea, dizziness, or insomnia - ask if an extended-release version is available.
- If you have trouble swallowing pills, tell your doctor. There may be liquid, patch, or smaller ER options.
- Never crush, split, or chew an ER pill. Ever.
- Check the label. If it says “XL,” “XR,” or “ER,” it’s not interchangeable with the regular version.
- If cost is an issue, ask about generic immediate-release. Sometimes the savings outweigh the side effects.
Medication form isn’t just packaging. It’s science. And it can make your treatment safer, easier, and more effective - if you know how to use it right.
Can I crush an extended-release tablet if I can’t swallow it?
No. Crushing an extended-release tablet can release the entire dose at once, leading to overdose or dangerous side effects. If you can’t swallow pills, talk to your doctor. Some ER medications come in liquid form, patches, or smaller tablets. Never assume a pill can be crushed - always check the label or ask your pharmacist.
Are extended-release medications always better than immediate-release?
Not always. ER versions reduce side effects like nausea and dizziness by smoothing out drug peaks, which helps many people. But they’re not ideal if you need flexible dosing, have digestive issues, or can’t afford the higher cost. For some, immediate-release works fine - especially if side effects are mild or manageable.
Why do some extended-release pills cost so much more?
Extended-release formulations require complex manufacturing, specialized materials, and longer development times - often 2.5 times more expensive to create than regular pills. Brand-name ER versions are especially pricey. Generic immediate-release versions often cost 70-90% less. Insurance may not cover ER unless you’ve tried and failed the cheaper version.
Do food and drinks affect extended-release medications?
Yes, sometimes dramatically. High-fat meals can increase drug absorption by 20-35% in 15% of FDA-approved ER products. For example, taking ER carbamazepine with a fatty meal can spike levels dangerously. Always check the label: some ER pills must be taken on an empty stomach, others with food. Never assume it’s the same as the immediate-release version.
What’s the difference between SR, XR, and ER?
These terms are often used interchangeably, but they’re not always the same. SR (sustained-release) usually means release over 6-12 hours. ER or XR (extended-release) typically means 12-24 hours. DR (delayed-release) means the drug doesn’t release until it reaches the intestine - like enteric-coated pills. Always check the specific drug’s prescribing information - the label matters more than the abbreviation.


Comments
Tablets take forever to break down. Capsules? Fast. ER? Slows it all down. Simple. No need to overcomplicate. If you can swallow it, fine. If not, ask for liquid. Done.
The hydrophilic matrix mechanism is fascinating-HPMC swelling into a gelatinous barrier is essentially a biocompatible time-release valve. The osmotic pump systems, like in Concerta, are engineering marvels. But let’s be real: most patients don’t care about the polymer chemistry. They care if they stop feeling like garbage after 3 days. And for many, ER delivers.
Bro, I used to crush my ER gabapentin like it was Adderall. Then I almost passed out. Now I just chug it with a banana smoothie. It’s not glamorous, but it works. Also, why do ER pills always look like they were molded by a toddler with a stress ball? Too big. Too hard. Too much.
I once had a doctor prescribe me ER sertraline because ‘it’s better.’ I asked why. They said, ‘It’s less side effects.’ I said, ‘What side effects?’ They said, ‘You’re not supposed to feel them.’ I said, ‘Then why am I crying in the shower?’ I switched back. Immediate-release. Smaller pill. Same drug. Different life.
I had no idea ER could cut nausea by 18%?! That’s huge 😍 I’ve been on venlafaxine for 2 years and thought the dizziness was just ‘part of it.’ Turns out, I just needed the XR version. My pharmacist even had a sample! So glad I asked. 🙌 Also, never crush ER pills-seriously, don’t. I’m not joking.
This whole post feels like a pharmaceutical ad. I take pills. I don’t care if it’s a matrix or a reservoir. Just give me the cheapest thing that doesn’t make me vomit.
Medication is not just chemistry. It’s dignity. It’s autonomy. It’s the quiet act of choosing to live, even when your body feels like a broken machine. The fact that we can engineer a pill to release slowly, gently, steadily-this is science serving humanity. Not profit. Not convenience. But care.
So let me get this straight. You’re telling me that the $185 pill is just a $15 pill with a fancy coat? And we’re supposed to be grateful? Meanwhile, my cousin in Nigeria is taking half-doses because she can’t afford the ‘XR’ version. This isn’t innovation. It’s a tax on being sick.
I work in pharmacy. I’ve seen patients swallow ER tablets whole, then immediately lie down. Bad idea. The pill can get stuck. Especially in elderly patients with esophageal motility issues. Always stay upright for 15-20 minutes. And if you’re struggling? Ask for the capsule form. Or liquid. Or patch. There’s always an option.
The environmental impact of polymer coatings in wastewater is something we rarely discuss. We treat pills like disposable items. But they’re not. They’re engineered polymers that don’t break down. We’re slowly poisoning the water we drink. We need better disposal systems. Or better formulations. Or both.
I don’t know why people act like ER is some miracle... I’ve been on it for 5 years. The side effects? They just... linger. Like a slow drip instead of a splash. So now I’m always tired. Always a little off. Maybe the problem isn’t the spike... maybe it’s the constant low-grade buzz. Just saying.
The assertion that extended-release formulations reduce side effects by 25% to 40% is statistically misleading. The cited studies often exclude patients with comorbidities, elderly populations, and those with non-adherence. A meta-analysis published in JAMA Internal Medicine in 2021 found no clinically significant difference in tolerability between ER and IR formulations in real-world settings. Marketing, not medicine.