That burning sensation in your chest after a spicy meal isn't just a nuisance-for about 20% of people in the U.S., it's a chronic condition called GERD is Gastroesophageal Reflux Disease, a chronic condition where stomach acid frequently flows back into the esophagus, causing inflammation and discomfort. When this happens more than twice a week, you're not just dealing with occasional heartburn; you're dealing with a systemic issue that can damage your esophageal lining over time if left unchecked.
The goal of managing this isn't just to stop the burn today, but to prevent long-term complications like Barrett's Esophagus, which can increase the risk of cancer. Whether you're trying to avoid lifelong medication or looking for a permanent surgical fix, there is a clear, stepwise path to getting your life back from acid reflux.
Step 1: The Foundation of Lifestyle Changes
Before reaching for a pill, most specialists suggest starting with Stage I management: your daily habits. The primary culprit in GERD is a weak or relaxed Lower Esophageal Sphincter (LES), the muscle valve that is supposed to keep acid in your stomach. If this valve doesn't close properly, acid escapes upward.
Simple changes in how you live and sleep can make a massive difference. For instance, elevating the head of your bed by about six inches uses gravity to keep acid down while you sleep. If you're overweight, losing even 10% of your body weight can lead to a 40% improvement in symptoms because it reduces the pressure on your abdomen. Similarly, avoid lying down for at least three hours after eating; hitting the pillow too soon after a big meal can increase reflux episodes by 50%.
You also need to address habits that actively relax the LES. Smoking and alcohol are major offenders. Nicotine can reduce LES pressure by up to 40% within just 20 minutes of a cigarette, and ethanol (alcohol) can drop that pressure by 25%. If you want the medication to actually work, these lifestyle tweaks are non-negotiable.
Identifying and Eliminating Dietary Triggers
Not every "healthy" food is good for GERD. For example, citrus fruits and tomatoes are naturally acidic (pH 2.0 to 4.6), which can directly irritate an already inflamed esophagus. But some triggers are more about how they affect your anatomy than their pH level. Peppermint and chocolate both contain compounds that relax the LES, making it easier for acid to slide back up.
Fatty foods are another huge trigger. When you eat a meal with more than 30g of fat, your stomach takes much longer to empty-sometimes 40 to 60 minutes longer than usual. This means food sits in your stomach longer, producing more acid and increasing the chance of reflux. Carbonated drinks also cause gastric distension, which increases the pressure inside your abdomen by up to 20 mmHg, essentially pushing acid upward.
| Trigger | Physiological Effect | Impact on Reflux |
|---|---|---|
| Caffeine (Coffee/Tea) | Increases gastric acid production by 23% | Higher acid volume |
| Fatty Foods | Delays gastric emptying by 40-60 mins | Prolonged acid exposure |
| Peppermint/Chocolate | Relaxes the LES by 10-20% | Easier acid backflow |
| Citrus/Tomato | Low pH (2.0 - 4.6) | Direct mucosal irritation |

Navigating Acid Reflux Medications
When diet and lifestyle aren't enough, you move into the medical phases of treatment. Not all medications work the same way; some are "band-aids" for immediate relief, while others are long-term regulators.
For quick, on-demand relief, antacids like calcium carbonate (Tums) are the go-to. They neutralize existing acid almost instantly, but the effect only lasts about an hour. If you need something longer-lasting but not as powerful, H2 Receptor Antagonists (H2RAs), such as famotidine (Pepcid), reduce acid production by about 60-70% and last up to 12 hours.
For moderate to severe cases, Proton Pump Inhibitors (PPIs) are the gold standard. Drugs like omeprazole (Prilosec) or esomeprazole (Nexium) shut down the acid-producing pumps in your stomach, reducing secretion by up to 98%. These are incredibly effective at healing erosive esophagitis-healing 80-90% of patients within eight weeks. However, timing is everything. To get the most out of a PPI, you should take it 30 to 60 minutes before your first meal of the day.
If PPIs aren't cutting it, there's a newer class called Potassium-Competitive Acid Blockers (P-CABs). The most notable example is vonoprazan (Voquezna). Unlike PPIs, P-CABs work faster and provide more sustained acid suppression throughout the night, which is a huge win for the 70% of PPI users who still experience "nocturnal acid breakthrough."
The Risks of Long-Term Medication
While PPIs are lifesavers for many, they aren't without risks when used for years. The FDA has warned that long-term use (over one year) is linked to a 30% increase in Clostridium difficile infections and a slightly higher risk of community-acquired pneumonia. There is also a concern regarding mineral deficiencies, specifically magnesium and vitamin B12.
Because of these risks, doctors now emphasize a personalized approach. Some patients may only need a "step-down" therapy where they use PPIs to heal the esophagus and then switch to a lower-dose H2RA for maintenance. Monitoring serum magnesium every six months is often recommended for those on long-term therapy to avoid serious deficiencies.
Surgical Options for Permanent Relief
When medications fail or you simply don't want to take a pill every day for the next twenty years, surgery becomes an option. This is Stage V of management. The most traditional approach is the Laparoscopic Nissen Fundoplication, where the top of the stomach is wrapped around the LES to tighten it. This has a success rate of 90-95% over five years, though some patients deal with "gas-bloat syndrome" afterward.
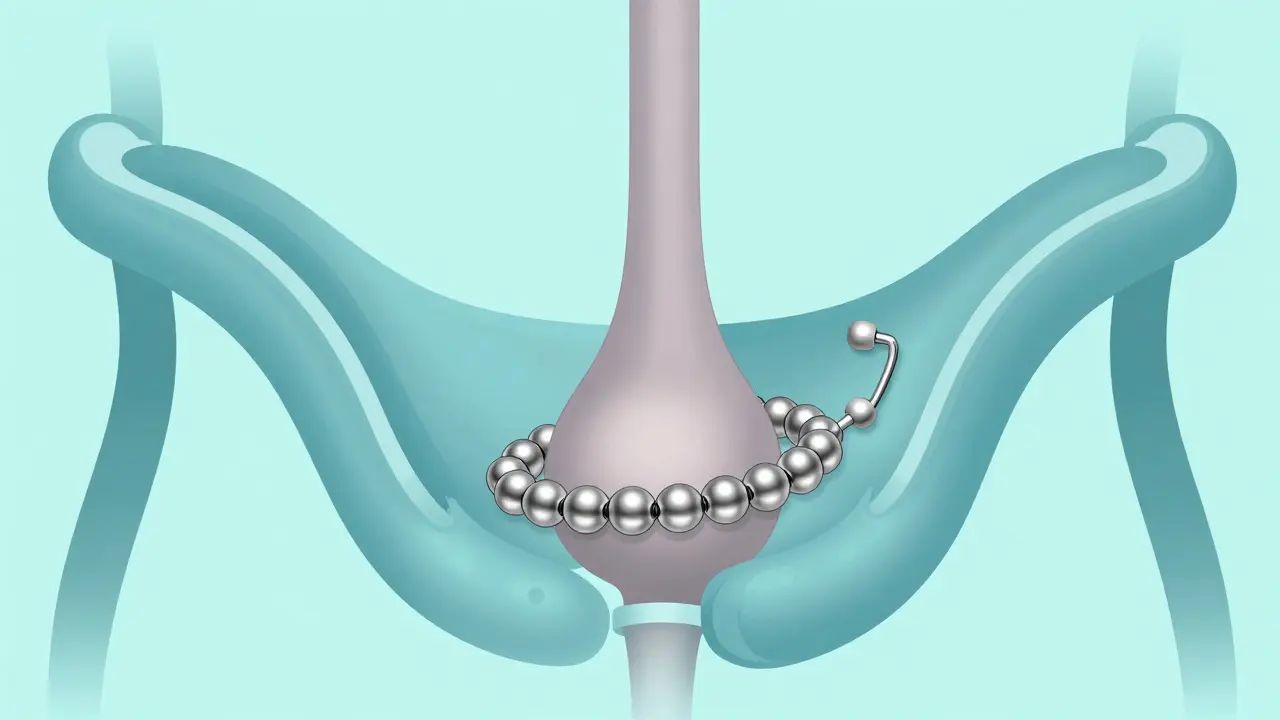
A less invasive alternative is the LINX Reflux Management System. This is essentially a small bracelet of titanium beads placed around the LES. It keeps the valve closed to acid but allows food to pass through. About 85% of patients stay off PPIs five years after the procedure. However, it's not for everyone-if you've had previous gastric surgery or need frequent MRIs, this might not be the right choice.
There is also a newer endoscopic procedure called Transoral Incisionless Fundoplication (TIF), which doesn't require external incisions. While it has a solid success rate, it's less common because it requires highly specialized training that only a small number of providers in the U.S. possess.
Practical Tips for Daily Management
Managing GERD is as much about data as it is about diet. Many people think they know their triggers, but they're often wrong. Keeping a food diary for 14 days-tracking exactly what you ate, when you ate it, and when the symptoms started-helps you identify the 2-3 specific foods that actually trigger your reflux.
Additionally, if you struggle with mild symptoms, try diaphragmatic breathing. Practicing this for 15 minutes after a meal can reduce symptoms by 35% by strengthening the muscles around the diaphragm and providing a natural buffer against reflux.
How long does it take for PPIs to start working?
While you might feel some relief within 1 to 4 hours, PPIs like omeprazole or esomeprazole require 2 to 5 days of consistent daily dosing to reach their maximum acid-suppressing effect.
Can I stop taking PPIs once my symptoms are gone?
You should never stop PPIs abruptly, as this can cause "rebound acid hypersecretion," where your stomach produces even more acid than before. Always work with your doctor to taper the dose slowly.
Is the LINX device better than Nissen Fundoplication?
It depends on your goals. Nissen has a slightly higher success rate in eliminating symptoms, but LINX is often preferred because it's less invasive and doesn't permanently alter the stomach's anatomy. However, LINX may cause some people to have difficulty swallowing large pills.
Why do some healthy foods like orange juice cause heartburn?
Citrus juices have a very low pH (between 2.0 and 4.0). When these acids hit an esophagus that is already irritated or inflamed from GERD, they cause a direct chemical irritation, regardless of how "healthy" the fruit is.
What is the difference between heartburn and GERD?
Heartburn is a symptom-the occasional feeling of acid rising. GERD is the chronic disease state where this happens frequently (usually more than twice a week) and can lead to permanent tissue damage.

Comments
makes a lot of sense
The section on diet is basic at best. Everyone knows about citrus and tomatoes. It's almost like the author thinks we've never heard of a trigger food before. This whole guide is just a rehash of a WebMD page from 2012 and doesn't offer anything groundbreaking.
The mention of P-CABs like vonoprazan is a crucial addition here because the pharmacokinetic profile is vastly superior for managing nocturnal acid breakthrough. I've noticed that the competitive inhibition of the H+/K+-ATPase pump is much more potent than the irreversible binding seen in traditional PPIs. It's interesting how the onset of action is accelerated, reducing the need for a long loading period. The reduction in gastric acid secretion is nearly absolute in some phenotypes. This really changes the game for patients who exhibit refractory symptoms despite high-dose omeprazole. The molecular stability of these compounds in various pH environments is what makes them so effective. We're seeing a shift toward more targeted acid suppression. It minimizes the rebound effect if managed correctly. The titration of these drugs requires a nuanced understanding of the patient's esophageal motility. This level of precision prevents the over-suppression of acid which can lead to SIBO. It's all about the balance of the gastric milieu. The transition from Stage IV to Stage V surgery is often delayed because P-CABs are so effective. The clinical data on these is promising. We are finally moving past the one-size-fits-all approach to reflux management.
The sheer horror of the rebound acid hypersecretion is just... unimaginable!!! Who thought it was a good idea to let our stomachs turn into acid factories??? The physiological trauma of a Nissen Fundoplication is literally a nightmare!!!
Elevating the bed really did work for me. It took a few nights to get used to the angle, but waking up without that bitter taste in my throat is a total win. Keep pushing through with the lifestyle changes, everyone!
my soul feels the burn just reading this lol!! it's like a wild dance between the stomach and the throat and we're just trying to keep the peace. maybe the universe just wants us to eat more oatmeal and vibe out with some deep breathin' and let the cosmic energy heal our tummies. just flow with it and stop fightin the acid tide!!
It's quite fascinating how they suggest these medications while ignoring the fact that the pharmaceutical industry has a vested interest in keeping us dependent on these pills because once you start the PPI cycle, your body's natural chemistry is essentially hijacked. I've spent years analyzing the patterns of these 'recommendations' and it's clear that the push toward surgical implants like LINX is just another way to monetize a biological function that was probably disrupted by the toxins they put in our processed foods in the first place, though I do wish everyone the best of luck in finding their own path to healing away from the mainstream narrative.
The advice regarding the timing of PPI administration is most accurate. Taking the medication thirty minutes prior to the first meal ensures maximal efficacy due to the activation of the proton pumps during the digestive process.